Compression Stockings: Used to promote blood flow and decrease the risk of developing blood clots in the legs.
CSS Considerations
- CSS should review the doctor’s order (from HCCSS or client).
- If the client’s health status changes or current orders are greater than 6 months old, a new doctor’s order should be requested.
- Determine appropriateness and safety of over the counter and prescribed stockings; both should be approved by a physician before PSWs are trained.
- Ensure that HCCSS is aware of over the counter stocking use; no delegation is
 required to apply these but CSS should still assess appropriateness.
required to apply these but CSS should still assess appropriateness. - Tubi-grip is not considered high level compression; no delegation/training is required for PSWs to apply, they are put on in the same manner as socks.
- Ensure that HCCSS is aware of over the counter stocking use; no delegation is
- Determine the number of pairs available for use and how often they are changed after use.
- Establish who applies and removes the stockings
- CSS to complete skin assessment, document and report abnormal findings
PSW Considerations
- Client must have 2 functional pairs
- Client is responsible for integrity of compression stockings and maintenance
- PSW should report to the CSS or call the office at 416-635-2860 to report any defects
How do compression stockings work?
- Compression stockings apply gentle pressure on the blood vessels in the legs and ankles, promoting blood flow back up to the heart
- They increase venous return and decrease venous resistance, making it easier for blood to flow back towards the heart
Benefits of compression stockings:
- Boosts circulation in the legs
- Supports veins
- Reduces pain
- Improves lymphatic drainage
Do not put on the stockings if:
- Skin breakdown: Open tears or cuts on the skin, any new wounds
- Infection: Hot to touch, swelling, pain, any drainage or pus
- Excessive swelling: Too tight to put on/remove, any new change in leg shape/ size
- Lack of sensation/feeling
- Any change in skin colour to lower legs and feet
Required Supplies:
• Compression socks
• Gloves
• Hand hygiene supplies
Procedure for Applying and Maintaining Compression Stockings
Application of compression stockings:
- Verify the clients care plan for application/removal of the compression stockings.
- Gather the necessary equipment and supplies.
- Perform hand hygiene and apply gloves.
- Inform the client when the procedure will begin, and remind the client when the stockings will need to be removed.
- Assess the skin integrity of the client’s legs. Do not apply compression stockings if the client’s skin integrity is compromised. The PSW should report to the CSS or the office at 416-635-2860 if the delegation cannot be completed.
- Ensure that the legs are clean. If needed, bathe and dry the legs.
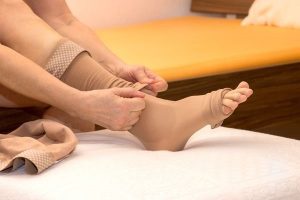
- Begin to apply the compression stockings by first turning the compression stockings inside out. Do so by placing your hand into the stocking as far as the heel pocket. Then pull the stocking inside out, but not all the way through.
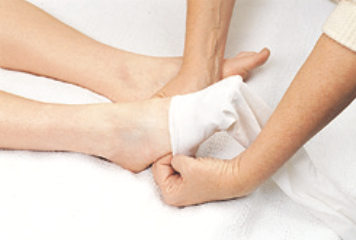
- Place the foot of the compression stocking over the client’s toes, making sure the stocking is smooth.
- Slide the remaining portion of the stocking over the client’s foot, keeping the heel in the heel pocket.
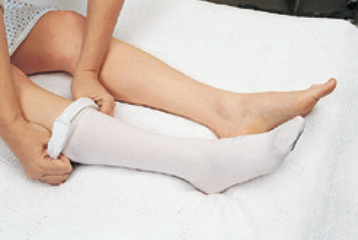
- Slide the stocking up until it is fully extended over the calf.
- Be sure that the stocking is smooth, with no wrinkles or creases.
- Make sure there are no toes overlapping or nails caught on the fabric.
- Repeat this process on the other leg.
- After completing both legs, remove and dispose of gloves if used. Perform hand hygiene.
Removing compression stockings
- Perform hand hygiene and apply gloves
- Hold the top of the stocking and begin turning it inside out; gently pull down to the ankle.
- Once at the ankle, put a finger in between the stocking and the foot and gently pull over the ankle.
- Slowly pull the stocking off the foot.
- Assess the skin integrity of the legs and feet for any abnormalities.
- Repeat this process on the other leg.
- Perform hand hygiene.
- Report any abnormal findings to the CSS/ office at 416-635-2860.
Skin Assessment
| Assessment | What to Look For |
| Colour | What is normal for the patient?
What colours can you see e.g. red, purple, unusual pigmentation of the lower limbs and gaiter regions (brownish) or blue/grey hues of distal limbs (lower limbs and feet)? Is there any bruising present? Or purpura? |
| Temperature | Does the skin feel cool to touch? (possibly due to poor peripheral perfusion) or hot due to fever or infection? |
| Texture | Does the skin feel dry or moist, papery, thin or leathery? |
| Moisture | Is moisture due to excessive sweating, urine or leakage from a wound or drain? Is the skin becoming macerated (white appearance)? Is oedema present? |
| Integrity | Are there any broken areas? Presence of skin tears, blisters, wounds, pressure injuries or epidermal stripping due to adhesive tapes or dressings? |
| Location | If there a failure in skin integrity, identify and document the anatomical location (i.e. sacrum, heels or toes, gaiter region of lower legs, dorsal/plantar surface of foot, groin or under skin folds and so on). |
Video Resource
Please click on the video link below for a visual demonstration of the procedure:
References
CareChannel. (2019, June 14). How to help with compression stockings – Tips for
caregivers [Video]. YouTube. https://youtu.be/Pf7uXvQ4kQk
Frothingham, S. (2019, August 7). What to Know About Compression Socks and
Stockings. https://www.healthline.com/health/compression-socks-benefits
Potter, P., Perry, A. G., Stockert, P., Hall, A. (2019). Canadian fundamentals of
nursing (6th ed,. Astle, B. J., & Duggleby, W. Eds.). Elsevier Canada.
Sigvaris Group. (2023). How to put on and take off compression stockings.
https://www.sigvaris.com/en-ca/expertise/how-to/put-on-and-take-off
